Pain in the neck, scapula, shoulder joint, and even chronic headaches and tinnitus can be caused by a herniated cervical disc, which accounts for 20-30% of all spinal hernias. A herniated cervical spine can be symptomatic of spinal cord compression or nerve root compression. Doctors are able to identify this problem and treat it successfully. It is important not to put off treatment for too long.
What is a herniated spine?
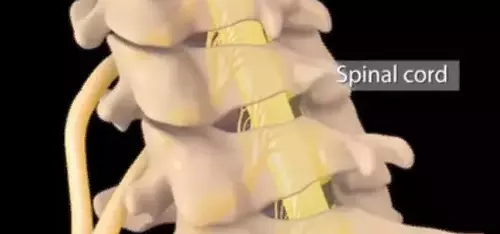
The cervical spine connects the thoracic disc to the skull. It consists of 7 vertebrae, consisting of a body and closed arches, within which the spinal cord passes. Because of the different structure of the two higher vertebrae, the cervical segment is the most mobile part of the spine. Forward, backward, side-to-side flexion/extension, and rotational movements can be performed. Because of this wide range of motion, the cervical spine is prone to damage and injury, which can contribute to hernias.
Between the vertebral bodies that make up the spine are the intervertebral discs, commonly known as discs. The disc consists of the central part, the jelly-like core of the pulp and the hard shell, the fibrous ring . When the ring is damaged due to, for example, trauma or degenerative changes, the nucleus pulposus can shift and cause:
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
- Rediculopathy – damage caused by chronic nerve root compression;
- Myelopathy – compression of the spinal cord.
What are the causes of a herniated cervical spine?
The main causes of a herniated cervical spine are:
- Degenerative disease of the intervertebral disc;
- trauma, the most common is whiplash injury , caused by a traffic accident in which there is an aggressive, voluminous and rapid movement of the neck, leaning forward, followed by pulling back;
- Overload caused by chronic, sometimes forced placement of the cervical segment in an improper position, such as when working at a computer.
- Most commonly, cervical discopathy is manifested by myelopathy of the shoulder or cervical spine. To diagnose a cervical hernia, a doctor or physical therapist performs a series of physical examinations and tests to assess neck and upper extremity mobility and symptoms indicating the height of the spine at which the hernia occurred. An additional imaging modality to diagnose a herniated cervical spine is an MRI scan.
Shoulder herniation of the cervical spine and herniated cervical spine
The most common sign of cervical rediculopathy is pain in the shoulder . The bulging nucleus of the intervertebral disc then presses on the nerve root, causing what is known as root symptoms . Depending on the level at which the cervical herniation occurs, the shoulder is characterized by:
- Pain in the neck and shoulder girdle, sometimes irradiating throughout the limb, increased by coughing, sneezing and certain head movements;
- Pain radiating from the back to the scapula;
- pain irradiating to the front of the chest (can be mistaken for a heart problem)
- tension in the neck and neck muscles that become tender when touched;
- muscle weakness in the upper extremity, especially if the problem has been going on for a long time;
- a tingling sensation in the upper extremity;
- other ailments such as: chronic headaches, tinnitus, visual disturbances.
Cervical myelopathy – symptoms of cervical spinal hernia
A bulge of the nucleus pulposus toward the spinal cord can cause cervical myopathy. Its symptoms are often bilateral.
They are:
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
- Pain in the spine and neck;
- weakness and impaired sensation in the neck, shoulder girdle, and along the upper extremity;
- paresthesia (tingling and burning) at the height corresponding to the level of injury;
- weakness and exhaustion of the muscles of the upper extremity (especially the muscles of the arm), which makes it impossible to hold an object in the hand
- impaired gait with spasmodic contraction of the muscles of the lower extremities;
- sexual dysfunction;
- urinary and stool incontinence.
Hernia of the cervical spine – prevention and treatment
If you experience symptoms that could indicate a herniated cervical spine, you should immediately see an orthopedist, neurologist, physical therapist or osteopath who is experienced in treating spinal conditions and pain. Failure to see a doctor in a timely manner can greatly aggravate pain, sensory and strength disorders, which can lead to upper extremity paresis.
To reduce the symptoms of cervical dyscopathy and avoid aggravation, you should:
- Minimize exposure to positions that cause and aggravate pain, exposure, and paresthesia;
- do not lift heavy objects;
- Do not make sudden movements of the neck and head;
- get plenty of rest. If possible, tilt your head so that the muscles in the neck and back of your head can rest. At night sleep on a specialized orthopedic pillow and a well chosen comfortable mattress;
- Use pharmacological treatment after consulting a doctor;
- Visit an experienced physiotherapist, who will competently conduct therapy using elements of manual therapy, massage, exercise therapy and physiotherapy.
What does cervical herniation seem like?
If you have actually a herniated cervical disc, you may feel pain that radiates down your arm and potentially into your hand. You might likewise feel pain on or near your shoulder blade, and neck pain when turning your head or flexing your neck. Often you might have muscle spasms (implying the muscles tighten up frantically).
How do you treat a neck hernia?
Many cases of cervical herniated disc pain can be effectively managed with nonsurgical treatments, such as non-prescription pain medications, physical therapy to strengthen and extend the neck, ice or heat packs, and/or activity modifications to avoid painful movements up until the pain has actually subsided.
Can cervical disc herniation be treated?
The good news is that most of the times — 90% of the time — pain caused by a herniated disc will disappear on its own within 6 months. Initially, your doctor will likely recommend that you take an over the counter painkiller and limit activities that cause pain or discomfort.
What happens if a cervical herniated disc goes without treatment?
If you leave a herniated disc neglected, you may experience extreme, acute pains, partial paralysis, or the failure to manage defecation in fairly dire situations.
Which is worse bulging or herniated disk?
Herniated discs are considered more severe than bulging discs due to the fact that they put significant pressure on neighboring nerves, which can cause extreme pain, swelling and problems with movement.
What are the symptoms of a herniated disc in the neck c5 and c6?
Symptoms of c5-c6 disc herniation can consist of numbness, tingling, burning, weakness, issues with vision, and more.
Can a chiropractic physician fix a herniated disc in neck?
9 out of 10 people with a herniated disc can heal their condition through non-invasive treatments. If you wish to explore conservative choices for recovery, chiropractic care is an exceptional place to begin. A chiropractic specialist can help you heal naturally and alleviate your pain.
How should I sleep with a herniated disc in my neck?
The optimum sleeping position for a herniated disc is on your back. Pushing your back keeps your spinal column in a neutral position so you have less possibility of pinching the nerve. For included convenience, nestle a small pillow or rolled-up towel under your knees and lower back.
Is walking good for herniated disc?
Definitely. Walking is an exceptional option for patients with herniated discs, as it promotes blood circulation and oxygen to the cells. It also helps keep your discs hydrated, which is very important for healing. Other low-impact aerobic activities to try are swimming and cycling.
How long does a herniated disc in neck require to heal?
Nevertheless, most symptomatic herniated discs end up fixing on their own. Some research studies show that cervical radiculopathy from a herniated disc can to begin feeling much better within 4 to 6 weeks, although some symptoms may last up to 6 months, and more than 80% of cases are symptom-free within 2 to 3 years.
Can you end up being paralyzed from a herniated disc?
The most severe complication from a thoracic herniated disc is the development of total paralysis listed below the waist. This results when a piece of disc product is burst into the spinal canal. Pressure on the spinal cord causes long-term damage to the nerves traveling to the lower body and legs.
Can a herniated disc not show on MRI?
MRI scan is the best non-invasive test available to find herniated and bulging discs and annular tears. Due to the fact that the spatial resolution of spine anatomy can be specified to 0.5 mm with an MRI scan, doctors can relate to over 95% precision the herniated discs in the spinal column.
Can herniated cervical disc cause memory issues?
Even symptoms such as fuzzy vision, changes in vision, ringing in the ears, vertigo, poor balance, brain fog, dystonia, tremblings, reduced memory, swallowing problem, hearing problems, and ear fullness, as well as any kind of cranial nerve problem, can be from cervical instability.
How do you fix a C5-C6 herniated disc?
Anterior cervical discectomy and blend (ACDF) surgery includes removing the C5-C6 intervertebral disc to ease pressure on the spine or C6 nerve root. The disc is changed by an implant or bone graft, permitting biological blend of the surrounding C5 and C6 vertebrae.
Can you push a herniated disc back into place?
The most crucial take-away here is to see a qualified doctor to diagnose your back pain and offer treatment alternatives. If you have back pain from a bulging disc, do not have your buddy try to require it back into place. This will likely increase, rather than relieve, your pain.
How do you sleep with a herniated c6-c7?
- Sleeping on your back: This is the ideal sleeping position as it is the easiest to properly brace your head and place your neck; or
- Sleeping on your side: This position is not as preferred as laying on your back, but it is much better than on your stomach.
Why is herniated disc even worse in the evening?
When resting on your back, the lower spinal column’s natural inward curve (called the back lordosis) is more emphasized than when sitting or reclining. Holding the spine in this position decreases the size of the passageways (foramina) where nerve roots exit the spinal column.