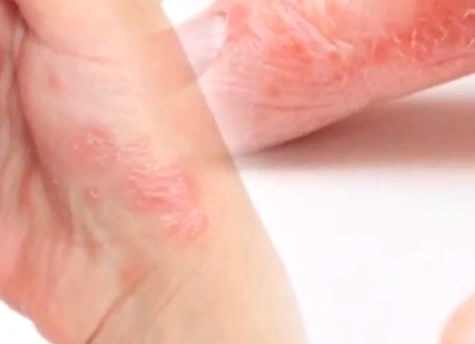
What is eczema? Causes, symptoms, diagnosis and treatment methods will be discussed in the article on iythealth.com
Definition
Eczema is a non-infectious chronic or acute inflammatory skin disease characterized by frequent relapses with itching, redness, and a fine rash in the form of blisters with fluid.
The word “eczema” means “boiling” in Greek. Indeed, the rash looks like bubbles of air when the water boils. Hence the name of the disease.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
According to statistics, about 10% of the world’s population suffer from some form of eczema. The disease affects people of all ages and is often caused by occupational factors. In eczema it is contraindicated to work in conditions of high humidity, associated with skin irritating and polluting agents, industrial allergens, so the disease often leads to a temporary disability.
Women get eczema more often than men. There is no exact explanation for this, but it may be due to working conditions, the influence of household allergens, and hormonal changes in the female body.
Recently, the number of cases of a severe course of the disease with frequent relapses and resistance to therapy has increased. This is due to the fact that modern man is surrounded by many allergens, uses synthetic materials, eats a lot of food additives and lives under stress with a constant lack of sleep and chronic fatigue.
Eczema is a non-infectious disease, so it cannot be transmitted from person to person. The disease is genetically conditioned and inherited: if one parent has eczema, there is a 25-40% chance that the child will also have it. If both parents have the disease, the risk rises to 50-60%. Therefore, heredity is the main cause of eczema. Eczema is characterized by multifactorial inheritance associated with many genes.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Causes of eczema
Eczema is a multifactorial disease and can be triggered by many factors.
The main causes of eczema are:
- Immune disorders;
- Allergic reactions to house dust, medications, plant pollen, household chemicals;
- endocrine disorders – disorders of the pituitary gland, adrenal glands, sex glands;
- stress, depression, nervous system disorders;
- foci of chronic infection – kidney inflammation (pyelonephritis), sore throat, otitis media and even dental caries;
- Diseases of the intestine, liver, pancreas, such as gall bladder inflammation (cholecystitis), gastritis, colitis, dysbacteriosis, stomach and duodenal ulcers;
- avitaminosis;
- hormonal disorders.
External factors such as:
- Temperature, such as hypothermia;
- Traumatization – mechanical impact, friction;
- Chemical agents, including cosmetic products;
- Foodstuffs and alcohol.
Various factors have a complex influence on the development of eczema: hereditary, endocrine, allergic and infectious.
Currently, the occurrence of eczema is considered as a pathological immune reaction, accompanied by damage and inflammation of body tissues. The main role is played by T-lymphocytes, cells involved in acquired immunity. They carry specific receptors on their surface and secrete a number of biologically active substances – pro-inflammatory cytokines. T-lymphocytes cause the development of inflammation in tissues, including an inflammatory response in the skin.
Thus, eczema occurs when provoking factors (chemicals, medications and microbial antigens in foci of chronic infection) and immune disorders combine. The body begins to produce antibodies-immunoglobulins-to its own skin cells, resulting in inflammation and the appearance of eczematous areas with blisters and redness.
An intercellular immunity disorder can be confirmed by laboratory diagnosis. In patients with eczema there are changes in glycoproteins: IgG and IgE immunoglobulin values are higher than normal, IgM is deficient.
Research also suggests that some people with eczema have a mutation in the gene responsible for creating filaggrin (a protein that helps maintain a healthy protective barrier of the epidermis). If it is deficient, the skin loses moisture, dries out and cracks, thereby opening the gates for bacteria and viruses. It is for this reason that many people with eczema have very dry skin and are prone to frequent infections.
Eczema symptoms
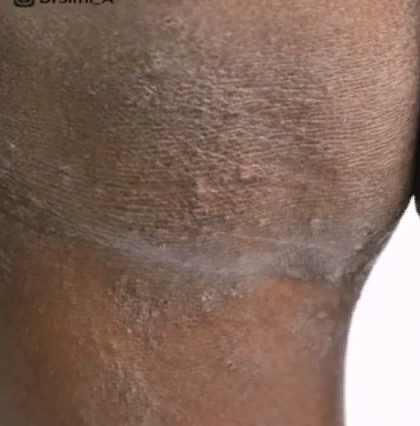
Eczema is characterized by sudden flare-ups and remissions. It can occur under the influence of triggering factors, but in a couple of weeks it goes away without a trace.
The main symptoms of eczema are:
- Severe to moderate itching;
- burning;
- Redness and swelling of the skin;
- A rash in the form of blisters.
Later, wet erosions, cracked skin, and then crusts appear. Yellow scales may localize on the scalp and eyebrows. In adults, eczema most often appears under the knees, in the elbow area, on the palms of the hands, and on the neck.
Although eczema can occur on any area of the skin, its favorite localization is on the hands and face. During bouts of exacerbation, eczematous lesions may appear in new areas. In children, the face, chest and chin are the most typical sites of localization of the rash.
The symptoms of eczema are individual, and each person has a different course of the disease. This is important to keep in mind when making a diagnosis. The patient may have a single symptom of the disease, or all together. And as practice shows, the clinical manifestations of the same type of eczema in two different patients will not be identical. The only sure way to find out if your skin problems are eczema is to make an appointment with a dermatologist. Do not self-medicate, as this can have negative consequences.
Itchness and Eczema
Itching is a form of skin sensitivity, close to touch and pain. But unlike the latter, which causes a withdrawal or avoidance reaction, itching produces a “processing” reflex. Scratching, rubbing, kneading, warming, pinching the itchy areas results in an immediate, but quickly passing feeling of comfort and reassurance. This is due to the fact that during the process of scratching, stronger impulses are simulated in the nerve endings, which suppress the conduct of weaker itching signals from the affected areas.
Severe itching is relieved only by severe self-injury, when the desire to scratch is replaced by a feeling of pain. If the itching torments a person for a long time, then a focus of pathological excitation is formed in the cerebral cortex, and from a defensive reaction, itching turns into a standard skin response to external and internal stimuli.
In eczema, itching ranges from mild to severe, and in some cases can become a major problem, affecting all members of the patient’s family, as it disrupts daily life and sleep.
Classification and stages of eczema
The following stages can be distinguished in the course of the disease:
- Erythematous – redness of the skin, swelling and itching appear.
- Papular – red papules (nodules) are formed.
- Vesicular – grouped blisters with liquid appear, resembling air bubbles when water boils.
- Blistering – the covers of the blisters open up and mucous membranes and erosions form.
- Cortical – pockets of mocculation dry up and become crusted.
- Exfoliation – the crusts peel off and the skin surface recovers.
When eczema progresses to the chronic stage, the skin changes: it becomes coarser and drier, and as a consequence, it peels and pigmentation appears.
Forms of eczema depending on the features of the clinical picture and the causes of occurrence:
- true;
- seborrheic;
- microbial;
- nummular;
- mycotic;
- intertriginous;
- varicose;
- sycosiform;
- Nipple eczema;
- pediatric;
- professional.
True eczema
True eczema most often affects the face and limbs. Areas of healthy and affected skin alternate. It may involve other areas up to and including erythrodermia (generalized inflammatory reaction and fever). The process is usually symmetrical. In the acute stage, the disease appears as vesicles (vesicles), skin redness, erosions with mucous, crusts, exoriations (mechanical damage to the skin when scratching), there may be papules and pustules. Eczematous lesions have irregular borders. When the disease progresses to the chronic stage, the redness becomes congestive, areas of cracking and lichenification (thickening of the skin with an increase in the skin pattern due to prolonged scratching) appear, the skin becomes rough and dry.Often the process is complicated by the appearance of pustules caused by the accession of infection: beta-hemolytic streptococcus or Staphylococcus aureus.
Nummular eczema
Nummular eczema occurs mainly in adults. Men fall ill more often than women. The highest incidence occurs between the ages of 50 and 65, and in both sexes. In women, the first peak is observed between the ages of 15 and 25, when puberty passes and women reach the height and weight of an adult. In children, on the other hand, nummular eczema is extremely rare. The lesions are often located at the elbow bends and under the knees, and the arms are affected more often than the legs.
The pathogenesis of the disease is still unclear. Some patients show foci of chronic infection, including in the oral cavity and respiratory tract. Allergens such as house dust mites play an important role in the development of nummular eczema. The disease develops clearly delineated coin-like plaques of papules and vesicles. Characteristic signs include fine-pointed blotches and crusts. The crusts may cover the entire plaque area, which varies in diameter from 1 to 3 cm. Itching may be either minimal or strongly pronounced. In ring-shaped forms of the disease, the manifestation decreases in the central part. Chronic plaques become dry, flaky, and the skin thickens.
Microbial eczema
Microbial eczema is a polyetiological disease. In the pathogenesis of microbial eczema, the skin barrier plays an important role, since one of its main functions is protection. Itching provokes skin scratching with damage to the integrity of the skin, and this, in turn, forms an entrance gateway for infection. Exudation (the exit of the liquid part of the blood into the inflamed tissue through the vascular wall) creates favorable conditions for the reproduction of microbes.
An important component of pathogenesis is the skin microbiota. In scrapings from the affected skin of patients with microbial eczema, golden and hemolytic staphylococcus aureus, yeast fungi, mainly of the genus Candida are found. Microbial eczema may also be caused by external physical or mechanical stimuli. Often foci of microbial eczema occur around purulent wounds and at sites of prolonged pyoderma (purulent skin disease due to infiltration of bacteria).
In microbial eczema, the lesions are round or irregular in shape, clearly delineated, asymmetrically and bordered by a border of peeling epidermis. Pus and serous crusts can be seen in the center of the lesions, and after their removal, a “well-like” mucous membrane is found. Rashes are characterized by intense itching.
Seborrheic eczema
Inflammation begins on the scalp and is localized in areas of the skin with most sebaceous glands. In this way, seborrheic eczema is similar to seborrheic dermatitis. The lesions localize behind the ears, on the chest, neck, between the shoulder blades, on the flexural surface of the limbs. The skin within the focus is hyperemic, edematous, with small papules of yellowish-pink color and fatty yellowish scales and crusts on its surface.
Varicose eczema
Varicose eczema, as the name implies, occurs when a patient has varicose veins. It mainly affects the skin of the lower legs in the vicinity of the varicose ulcers. It is caused by inadequate or untimely treatment of the varicose ulcers, maceration of the skin (skin wrinkling due to prolonged contact with water) and trauma. In varicose eczema, severe itching is noted. The differential diagnosis should primarily be made with myxedema and hornblastitis.
Sycosiform eczema
The disease occurs against the background of vulgar sycosis – inflammation of the hair follicles as a result of the penetration of staphylococci into them. The pathological process can extend beyond the boundaries of the hair, as a rule, foci can be found on the upper lip, in the armpits, on the chin and pubis. Clinically, sycosiform eczema is manifested by serous wells, pronounced itching and mucous, and later there are areas of skin thickening.
Pediatric eczema
The first symptoms can be noticed at the age of 3-6 months. The eczematous areas are symmetrical, the skin within the foci is brightly hyperemic, swollen, hot to the touch, has a shiny smooth surface, and there is mucous, overlapping and milky crusts. Eczema mainly affects the cheeks, forehead, scalp, ears, buttocks and extremities (usually the extensor surfaces). Characteristically, eczema does not affect the skin of the nasolabial triangle. Children complain of itching and insomnia. It is not uncommon for eczema to transform into atopic dermatitis.
Eczema of the nipples of the mammary glands
The skin disorder occurs after nipple trauma during breastfeeding. Externally, eczema appears as slight redness, mottling, crusts of blood accumulation, and in some cases pustules and fissures, usually without nipple thickening. The eczematous process usually spreads to both breasts.
Occupational eczema
It occurs under the influence of various occupational allergens. The disease can be caused by mercury, various metal alloys, penicillin and semi-synthetic antibiotics, resins and synthetic adhesives. Occupational eczema is more common among workers in different industries, people who deal with different chemicals (chemists and biologists) and those whose work involves constant immersion in water (for example, cleaners and sanitation workers). Under the influence of allergens, a delayed hypersensitivity reaction develops. Clinically, occupational eczema runs like ordinary eczema. The lesions are mainly in contact with the allergens and on exposed skin. Occupational eczema is characterized by a rapid recovery, once the cause is removed.
Paratraumatic eczema
It occurs in the area of postoperative scars or improperly applied plaster casts. It manifests as erythema osteoinflammatory (redness), pustules or papules, and crusts. Hemosiderin, a yellow pigment formed during hemoglobin decomposition, can be deposited in the affected tissues.
How dangerous is eczema to humans?
Eczema can be complicated by pyogenic infection caused by beta-haemolytic streptococcus, Staphylococcus aureus and gonococcus. The development of purulent inflammation results in a soggy surface with a putrid odor. This affects the general well-being – malaise and fever appear.
Another serious complication of eczema is erythroderma, in which the inflammatory reaction affects up to 90% of the skin surface. The disease is triggered by provoking factors, such as medications, stress, irrational treatment or exacerbation of chronic diseases. Erythroderma has a high body temperature and a high mortality rate.
Diagnosis of eczema
The identification of eczema is based on the collection of history, clinical manifestations and laboratory tests.
For diagnosis, the following are performed:
Blood tests:
- liver tests;
- triglycerides;
- glucose;
- bilirubin profile;
- IgE antibodies.
Also:
- Urinalysis.
- Skin tests for allergens.
- Determination of antibodies to parasite antigens.
For differential diagnosis, histology of skin biopsies (biological material obtained by biopsy) is performed.
Occupational eczema is detected by skin tests with suspected irritants: mercury, metal alloys, penicillin and semi-synthetic antibiotics, resins and synthetic adhesives. If necessary, consultations with allied medical specialists (therapist, endocrinologist, allergist, gastroenterologist) are prescribed.
True eczema is important to differentiate with atopic dermatitis, pyoderma, allergic contact dermatitis, and toxicoderma.
Atopic dermatitis is characterized by family history of allergic diseases, susceptibility to atopy (bronchial asthma, pollinosis), disease onset in the first year of life, marked dry skin, seasonality of exacerbations (autumn-spring).
True eczema is distinguished from pyoderma by the symmetry of the lesions and their lack of clear boundaries.
For allergic contact dermatitis to develop, repeated or prolonged exposure of the skin to an irritant is necessary to provoke an immune response and specific inflammation of the skin. Most often the foci of inflammation are located on exposed areas of the body in contact with the irritant, and are not always symmetrical in nature, unlike true eczema.
The clinical picture of toxicoderma is polymorphic: the elements range from inflammatory spots and papules to blisters, pustules and nodules. The inflammatory elements have different shapes, sizes, shades, and are more often symmetrically located throughout the skin.
Coin eczema is similar to rosacea, plaque parapsoriasis and seborrheic eczema, with nodules with whitish scales on the surface. The nodules are predominantly on the abdomen, back and chest.
In microbial eczema, a differential diagnosis is made with contact allergic dermatitis and streptoderma. Streptoderma is characterized by infection after close contact with a sick person. In some cases, streptoderma is accompanied by an increase in body temperature and an increase in lymph nodes.
Dyshydratic eczema (a disease with rashes in the form of serous blisters of small size) must be distinguished from dermatomycosis, palmar and plantar psoriasis, chronic acrodermatitis allopo.
Dermatomycoses are fungal skin diseases that can be caused by poor personal hygiene, internal diseases, or taking certain medications (hormones, antibiotics, cytostatics).
Treatment of eczema
Eczema is a chronic genetically determined disease, so it cannot be cured forever. The goal of therapy is to achieve remission, improve quality of life and prevent new symptoms. Specific treatment is individual for each patient and depends on the clinical manifestations and form of eczema.
For the elimination of symptoms are prescribed:
- antihistamines tablets, during the acute stage of the disease use antihistamines of the first generation;
- pharmacy moisturizing creams to restore the water balance of the skin;
- hormonal ointments (glucocorticosteroids) – in the presence of a strong inflammatory reaction;
- Topical corticosteroids;
- tranquilizers with antihistamine action – in case of severe skin itching;
- antibiotics – in the presence of microbial eczema, accession of secondary infection with high body temperature;
- retinoids – in tylottic or horny eczema with evident infiltration (accumulation of cellular elements with blood and lymph in the tissues) and hyperkeratosis (thickening of the stratum corneum);
- solutions of tannin, silver nitrate, boric acid, “Cindol” for a week – as lotions;
- external antiseptics for 1-2 weeks (brilliant green or Fucorcinum) – for treatment of rashes.
With severe exudation detoxification is carried out – intravenous sodium thiosulfate, calcium preparations, as well as antihistamines are used. Exudation is the exit of the liquid part of the blood through the vascular wall into the inflamed tissue.
In some cases a good complementary treatment is light therapy – apparatus therapy with dosed exposure to light from artificial sources with certain wavelengths.
Patients are also often prescribed physical therapy-ultraviolet therapy with a wavelength of 311 nm, a course of 25-30 procedures.
Eczema patients are advised to avoid eggs, citrus fruits, seafood, fatty fish, rich broths of meat, whole milk, nuts, carbonated drinks, and alcohol.
10 Tips for Eczema Itch Relief
- Use sulfate-free skin cleansers (oils, “soap without soap”).
- For very severe itching, apply a cold compress for a while.
- Caress the itchy skin, not scratch it.
- Wear soft, breathable clothing without synthetic fibers or high wool content.
- Moisturize your skin daily.
- Antihistamines don’t always stop itching, but they can help people with eczema sleep.
- Wear thin cotton or viscose gloves at night to prevent scratching the skin in your sleep.
- Cut your nails short, so they damage your skin as little as possible.
- Ventilate the room you are in for extended periods of time daily, use an air purifier and humidifier.
- Avoid stressful situations.
Prognosis
With timely adequate treatment, as well as compliance with the prescribed recommendations of the doctor, the prognosis is favorable.
For remission to be prolonged, it is necessary to eliminate the external causes that led to the disease. It is important to remember that in some cases, eczema manifests itself some time after exposure to the triggering factor, and it can be problematic to track it down.
Sensitization occurs the first time the allergen comes into contact with the body. This is the “activation” of the immune system, the formation of a specific reaction to the irritant, which may not manifest itself externally. When the allergen acts again, the immune system “recognizes” it, and an immune response develops, manifesting as specific inflammation on the skin.
Causes of eczema flare-up
A flare-up of chronic eczema can occur for several reasons:
- In close contact with flower pollen. Some people have sensitive enough skin that they react instantly to such allergens.
- Increased sweating.
- Stressful situations that lead to strong worries or even nervous breakdowns.
- Changes in the body related to the work of the immune system.
- As a result of taking certain medications that cause similar adverse reactions.
- As a result of eating certain foods that cause allergic reactions.
Dealing with the question of how to treat eczema, first of all it is necessary to determine the exact list of causes that triggered the exacerbation of this chronic disease. This is a prerequisite for effective therapy.
What to do when eczema worsens
The treatment of eczema is carried out on an individual basis, after a diagnosis has been made. Most often a special hypoallergenic diet is prescribed, excluding from the patient’s diet foods that can provoke allergic reactions.
To get rid of the effects of this pathology, doctors prescribe certain ointments to treat the affected areas of the skin.
As a rule, the treatment process involves the use of hormonal creams and ointments, the task of which is to reduce inflammation and rapidly heal wounds or cracks that have already formed.
Prevention
To minimize the risks of eczema, it is important to adhere to the following guidelines:
- If prone to inflammation of the epidermis, do not overdry the skin;
- Do not overdry your skin, and do not drink too much;
- Do not abuse hot baths and showers;
- adhere to a healthy diet, exclude alcohol, coffee, citrus fruits, smoked foods, and spicy foods;
- Use household chemicals with caution.
Eczematous lesions should not be scratched to prevent them from spreading further. You should also avoid contact with irritating materials. Clothing should prefer soft, breathable fabrics, preferably made of natural cotton or linen. Clothes made of wool and artificial silk should be avoided in the case of eczema, since they cause itching.
Q&A: Expert answers…
Is eczema contagious?
No.
Can eczema go away on its own, without treatment?
Since it is a chronic skin disease, it can subside for a while, but sooner or later a period of exacerbation will return. Unfortunately, many people self-treat – use some ointments, tinctures. This is something that should not be done with eczema. You should be treated by a dermatologist – only he can make the right diagnosis and prescribe adequate treatment. Self-treatment can often lead to serious complications.
How is eczema treated?
Patients of any age should follow a hypoallergenic diet – that is, exclude from the diet foods that may be triggers of the disease. For adults, this includes alcoholic beverages, compotes, juices, lemonade, products with dyes, preservatives, candy, chocolate, honey, jam, berries, imported fruits.
Patients should try to avoid stress. They are advised to examine the gastrointestinal tract – often reveal problems with the liver, stomach. They should not come in contact with chemically active substances (including synthetic and chlorinated detergents).
Treatment consists of prescription of desensitizing, antihistamines, antibiotics may be used for microbial eczema.
Eczema may be treated with lotions, such as a solution of MiraMistin or Rivanol, pastes, creams, etc. Hormone-containing medications are used exclusively under the supervision of a doctor.
Can I swim at the beach with eczema?
There is a myth: If an eczema sufferer swims in the sea – especially in the Dead Sea, he will be cured immediately. No way! When exacerbated, it is generally not advisable to swim in the sea: exposed inflammatory foci react to the salt in the sea water, and the itching, rash intensifies. If you go to the sea in remission – when there are no rashes, it has a beneficial effect on the prevention of all skin diseases.
Is it possible to prevent the development of eczema, and if so, how?
Prevention is possible. It is necessary to normalize the regime of the day, to eat rationally, if possible, control the work of the nervous system.
Conclusion
See a dermatologist if the itching and redness you are experiencing does not go away on its own or if it interferes with your life. A skin doctor, called a dermatologist, can diagnose and treat eczema.
To help your doctor understand your condition, it may be helpful to keep a diary to identify eczema triggers. Record:
- what you eat and drink
- what skin products, chemicals, soaps, cosmetics and detergents you use
- things you do, such as hiking in the woods or swimming in a chlorinated pool
- how much time you spend in the bathtub or shower and what the water temperature is
- when you are stressed.
You should begin to notice the connection between your activities and your eczema flare-ups. Bring this journal to your doctor to help him or her pinpoint the triggers of eczema, determine its type and stage, and, then, prescribe treatment.