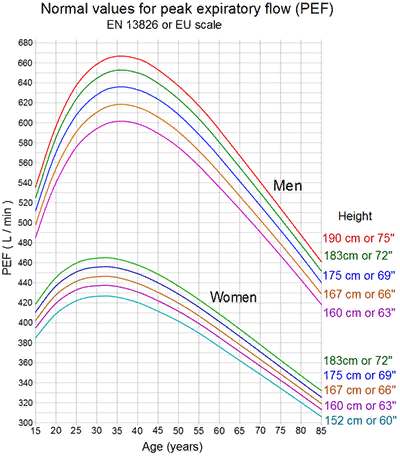
Rare clinical disorder characterized by air in the mediastinum; sometimes called mediastinal emphysema or pneumomediastinum. The heart, tracheobronchial tree, and esophagus all reside in this area between the lungs.
Pneumomediastinum air may go to the cervical subcutaneous tissues, the pericardium, the epidural space, and the peritoneal cavity from the esophagus, trachea, and lungs.
Pneumomediastinum may develop for no apparent reason, or it might have a secondary cause like trauma. The most prevalent cause of this disease is alveolar rupture. Inhalation of recreational drugs, chronic vomiting, forceful inhalation or sneezing, and persistent, violent coughing are all associated with an increased risk of spontaneous pneumomediastinum.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Pneumomediastinum is often self-limiting and very occasionally life-threatening; therefore, diagnosis and treatment concentrate on relieving symptoms and ruling out more severe causes.
Causes
Damage to the respiratory system (including the lungs and airways) or the digestive system (including the colon) may all lead to this illness. Alveolar rupture may cause pneumomediastinum, which can occur in a patient with a history of chronic obstructive pulmonary disease (COPD) who has a significant coughing fit. A patient might also develop air leakage into the mediastinum if they swallow a foreign item that becomes trapped in their esophagus.
Symptoms of Mediastinal Emphysema
Below are some of the most often seen signs of mediastinal emphysema:
- Pain below the breastbone or sternum that is severe enough to cause discomfort while breathing or swallowing
- Little air bubbles or pockets of air may be felt just beneath the surface of the skin on the chest, arms, and neck in people with subcutaneous emphysema.
- The buildup of air in the mediastinum may cause either a distorted or excessively high-pitched voice.
- Breathing problems, such as shortness of breath, may arise under extreme circumstances or when the underlying reason is potentially fatal.
Mediastinal Emphysema vs. Pneumothorax
While mediastinal emphysema may have no outward signs, it may produce excruciating chest discomfort that spreads to the shoulders and arms. Breathing or swallowing may aggravate the discomfort.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Pneumothorax, in which air enters the pleural cavity from somewhere other than the lungs, should be distinguished from mediastinal emphysema. Both illnesses are characterized by an excess of air inside the chest, but they are diagnosed and treated differently. Pneumothorax is characterized by the rapid onset of chest discomfort, shortness of breath, and diminished lung sounds on the side of the pneumothorax. Yet, mediastinal emphysema is often characterized by a crepitus or “crackling” feeling upon chest examination.
Diagnosis
An X-ray or CT scan of the chest may confirm the diagnosis. Doctors sometimes report feeling tiny air pockets beneath the skin of the chest, arms, and neck while doing a medical examination. As breathing in air is normally a slow process, it may not be necessary to undergo treatment. Pneumothorax, for instance, may result from chest trauma, whereas mediastinal emphysema might manifest itself in the face of a severe respiratory infection. Imaging investigations are useful for diagnosis and therapy planning in both circumstances.
Treatment
If the air is not being taken in, medical attention may be necessary. Sometimes, the body may just take in the air without any help from outside sources.
High quantities of oxygen and chest tube implantation may be employed to facilitate quicker absorption in emergency situations. The prognosis of pneumomediastinum is related to the etiology of the illness.
If you have chest discomfort and are having trouble breathing, you should get medical help right away. The ailment itself may not be life-threatening, but the underlying causes often are.