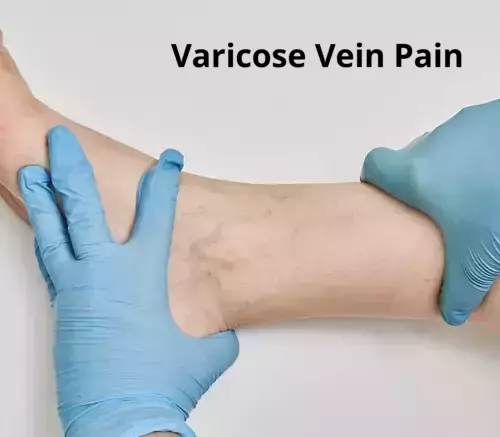
Varicose vein pain is a widespread issue that affects millions of individuals worldwide, particularly in their lower extremities. These enlarged, twisted, and bluish veins result from weak or damaged vein walls and valves, leading to impaired blood flow.
Symptoms of varicose vein pain may include aching, heaviness, itching, and skin changes around the affected veins. This discomfort can significantly impact an individual’s daily activities and overall well-being, making it crucial to understand the causes, symptoms, and treatment options for this prevalent condition.
Causes of Varicose Vein pain
Varicose vein pain is often caused by weakened or damaged valves within the veins. These valves prevent blood from flowing backward, however, when they become impaired, blood can pool and cause the veins to stretch or twist. Factors contributing to the development of varicose veins include aging, hormonal changes in women, and genetic predisposition. Symptoms can range from mild to severe, with some individuals experiencing phlebitis or blood clots, leading to inflammation and intense pain.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
After walking and exercise
Many individuals often experience leg pain during or after exercise, dismissing it as muscle fatigue. However, such discomfort can indicate an underlying circulatory issue called venous insufficiency. Symptoms include blue or purple-colored spider veins, bulging varicose veins, leg ulcers, and feelings of achiness, itchiness, and cramping. Venous insufficiency occurs when leg veins struggle to return blood to the heart during workouts, causing blood to pool in the lower extremities. Low-impact exercises, like walking, can help alleviate pain and improve circulation.
At night
Many individuals who suffer from varicose veins experience significant pain and discomfort at night, which can greatly impact their quality of sleep. This nighttime pain can often be attributed to the presence of venous insufficiency, a condition that causes blood to pool in the veins, leading to swelling and inflammation. Additional factors contributing to varicose vein pain at night include increased physical activity during the day, prolonged periods of sitting or standing, and other existing chronic conditions such as arthritis. Thankfully, numerous treatment options exist for those suffering from varicose vein pain, offering much-needed relief and improved quality of life.
All day
Varicose veins can cause pain in the form of a heavy or deep ache, particularly during warm weather, late in the day, or after standing for long periods. Inflammation, blood clots, and damaged lymphatic systems can lead to more severe pain. Complications like cellulitis, venous stasis dermatitis, and superficial thrombophlebitis arise from varicose veins and can also cause pain. To alleviate symptoms, experts recommend exercise, avoiding long periods of standing or sitting, and wearing compression stockings.
Treatment Options for Varicose Vein Pain
- Self-care measures: Exercise and elevate legs when sitting or lying down.
- Compression stockings: Wear these to help with blood flow and alleviate pain.
- Sclerotherapy: A noninvasive procedure to close problem veins.
- Laser treatment: Light energy used to make veins disappear.
- Catheter-based procedures: Heat used to collapse and seal veins.
- Vein stripping: Tying off and removing problem veins.
- Ambulatory phlebectomy: Smaller veins removed through tiny skin punctures.
- Maintain hydration: Helps with blood circulation.
- Cold water showers: Constricts blood vessels, reducing swelling and heaviness.
Preventive Measures for Varicose Vein Pain
Varicose vein pain can be debilitating for sufferers, but there are various preventive measures that can be taken. Elevating the legs, flexing the feet, staying hydrated, and applying cold water can provide immediate relief. Wearing compression hosiery and comfortable clothing, as well as avoiding prolonged sitting or standing, can address underlying issues. Early treatment and regular consultation with a doctor can help manage this condition more effectively.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Varicose Vein Pain in Pregnant Women
Varicose vein pain during pregnancy is a common concern affecting up to 80% of pregnant women due to hormonal and mechanical changes. The increased levels of estrogen and progesterone, along with pressure from the uterus, often lead to venous insufficiency and painful varicose veins. Treatment options include compression hose, leg movement, and elevation to reduce pressure on the veins. After pregnancy, advanced treatment procedures like sclerotherapy and radiofrequency ablation can be considered for persistent cases. Overall, effective management and monitoring of varicose vein pain contribute to improved comfort and health for expecting mothers.
Potential Complications of Varicose Vein Pain
Varicose vein pain, if left untreated, can lead to several complications that adversely impact an individual’s health and well-being. Potential issues include blood clots, either superficial or deep vein thrombosis (DVT), which can be life-threatening, bleeding from surface veins, chronic leg ulcers caused by vein problems, and lipodermatosclerosis, wherein the skin and fat harden, restricting mobility. Timely treatment and regular monitoring of varicose veins are essential to prevent such complications.
Self-Care Measures to Manage Varicose Vein Pain
Dealing with varicose vein pain can significantly impact one’s daily life. Thankfully, various self-care measures can help manage this discomfort and improve overall vein health. These measures include wearing compression stockings, engaging in low-impact exercises, elevating the legs, and maintaining a healthy diet rich in fiber and potassium. By adopting these simple yet effective practices, individuals can effectively alleviate varicose vein pain and promote better circulation for optimal well-being.