What is it? Your blood goes from your heart to your lungs through your pulmonary artery. In the lungs the blood is supplied with oxygen, then it returns to the heart, which pumps the oxygen-rich blood to the rest of your body.
When an embolism gets captured in one of the arteries that go from the heart to the lungs, it’s called a pulmonary embolism (PE). The clot obstructs the normal circulation of blood.
This blockage can trigger serious issues, like damage to your lungs and low oxygen levels in your blood. The lack of oxygen can damage other organs in your body, too. If the clot is big or the artery is clogged by numerous smaller sized embolisms, a pulmonary embolism can be deadly.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Main Causes of Having Blood Clots in Lung
Pulmonary embolisms typically move to the lungs from a deep vein in the legs. Physicians call this “deep vein apoplexy” (DVT). These embolisms develop when the blood can’t flow freely through the legs due to the fact that your body is still for a long period of time, state throughout a long flight or drive. It may also take place if you’re on bed rest after surgery or illness.
What Else Could Raise My Chances of PE?
The danger factors are the exact same as those for DVT. Medical professionals describe these as “Virchow’s triad.” They include:
- Being immobile for a prolonged amount of time or having changes in normal blood flow. This typically occurs if you’ve been hospitalized or on bed rest for a long period of time. It might also take place during a long flight or vehicle flight.
- Increased clotting potential of your blood. Medical professionals call this “hypercoagulability.” This might be caused by medications, like birth control pills. Smoking cigarettes, cancer, current surgery, or pregnancy can also put you at threat.
- Damage to a capillary wall. Trauma to your lower leg can result in this.
In rare cases, an artery in the lung can be obstructed by something aside from a clot, like an air bubble or part of a growth. If you break a huge bone, in some cases fat from the bone marrow can come through the blood and cause obstruction.
In lethal cases of pulmonary embolism, your doctor might decide to give you drugs called thrombolytics to break up the clot. It might even require to be taken out or broken up with surgery, though this is unusual.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
Symptoms of Pulmonary Embolism
When an artery in your lung gets blocked by a blood clot, you have a pulmonary embolism.
Symptoms can vary. What you experience will likely depend on the size of the clot and just how much of your lung it impacts. If you have lung or heart problem, that can contribute, too.
PE Is a Medical Emergency
Symptoms of PE tend to come on unexpectedly. Call 911 if you have any of the following:
- Shortness of breath
- Chest pain
- Cough (it may be bloody, and there may be blood in the gunk you cough up).
- Pain in your back.
- A lot more sweating than usual.
- A lightheaded sensation, or passing out.
- Blue lips or nails.
Indication of Deep Vein Thrombosis
When a clot types in a deep vein in your legs, it’s called deep vein thrombosis (DVT). If it breaks off and takes a trip to your lung, it ends up being a PE.
See your doctor immediately if you have any of the symptoms of DVT. If it’s discovered early, medical professionals can stop it from ending up being a pulmonary embolism. Signs of DVT include:
- Swelling of a leg or arm.
- Leg pain or inflammation when you’re standing or walking.
- A swollen leg or arm that feels warmer than normal.
- Red or blemished skin in the affected arm or leg.
- Veins in your arm or leg that are bigger than normal.
How Do Doctors Diagnose a Pulmonary Embolism?
If you believe you have a pulmonary embolism (PE), you must get medical aid immediately.
Your doctor will likely begin with a physical examination. He’ll look carefully at your legs to see if they’re swollen, tender, discolored, or warm. These are signs that you may have a clot deep in among your veins.
Next, your medical professional may order a variety of tests, like a chest X-ray or ultrasound. You may likewise have blood tests. These can measure the amount of oxygen and co2 in your blood. They can also assist your doctor discover a compound called D dimer. This is a small protein fragment that’s present in the blood after a clot is broken down by the body.
Other tests your medical professional might purchase include:
- Computed tomographic angiography (CTPA). This is a special type of X-ray test. It’s also the primary one doctors utilize to see if you have a PE. Your physician will inject dye (” contrast”) into your veins. He’ll be able to see the blood vessels in your lungs on the X-ray.
- Ventilation/perfusion (V/Q) scan. This test is used if the CTPA isn’t readily available, or isn’t a good match for you. It uses a radioactive product to show which parts of your lungs are getting air circulation (ventilation) and blood flow (perfusion). If there’s low blood flow to a specific area, however the air flow is normal, a clot may exist.
- Pulmonary angiography. This is the most precise test to spot PE. It may be utilized if other tests have not revealed clear outcomes. A professional inserts a long, thin tube (catheter) into a big vein in your groin and into the arteries within your lung. He then injects dye through the catheter. Pictures of the blood vessels inside the lung will turn up on an X-ray.
- MRI. This might be a good choice if you’re pregnant or your medical professional is worried that other tests that utilize contrast might be damaging to you.
- Echocardiogram. This is an ultrasound of the heart. It can’t identify a PE, but it does show if you have stress on your heart triggered by one.
What’s the Treatment for a Pulmonary Embolism?
A pulmonary embolism (PE) is an embolism in the lung. It’s serious and can be dangerous. However fortunately is that if it’s captured early, doctors can treat it. Here’s a take a look at a few of the most typical ways they tackle this condition.
Blood Thinners
Also called “anticoagulants,” these are the most typical treatment for a blood clot in the lung. They serve 2 key roles: First, they keep the clot from getting any larger. Second, they keep new embolisms from forming.
They do not dissolve blood clots. Your body typically does that by itself gradually.
The most commonly recommended blood thinners are warfarin (Coumadin, Jantoven) and heparin. Warfarin is a pill and can deal with and avoid clots. You get it through a shot or an IV. There are numerous other blood thinners in pill type, and your physician will help decide which agent would work best in your situation. Heparin can lower the opportunities of another clot forming. You get it through a shot or an IV.
Treatment can begin while you’re in the healthcare facility or even in the ER and you can be discharged the exact same day. How long you’ll remain and be treated depends on your condition.
Low-molecular-weight heparins are also extensively utilized. These can be self-injected at home. They include:
- Dalteparin (Fragmin).
- Enoxaparin (Lovenox).
- Tinzaparin (Innohep).
Internal bleeding is the main adverse effects of blood thinners. It can take place if the medicine thins your blood excessive. Your medical professional may give you blood tests to keep an eye on that. However, even when at healing dosages, internal bleeding remains a risk.
In dangerous situations, physicians might use what are called thrombolytic drugs. These rapidly separate clots that trigger serious symptoms. However they can cause sudden bleeding and are just used after mindful consideration.
Catheter
In carefully picked cases, his is another first aid your medical professional may use. He’ll insert a thin, flexible tube into a vein in your thigh or arm. He’ll advance to your lung, where he’ll eliminate the embolisms or use medicine to dissolve it.
Other Treatments
If you can’t take blood thinners, your doctor may use these choices to treat your PE:
- Inferior vena cava filter. The inferior vena cava is a big vein that brings blood from the lower body to the heart. Your doctor can put a filter in it to stop embolisms before they get to your lungs. It won’t stop embolisms from forming – just from getting to the lungs.
- Compression stockings. Sometimes called “support hose pipe,” compression socks go up to your knee and keep pressure on your legs so blood doesn’t pool or clot. (Most embolisms that end up in the lung start in the leg.).
- Surgery. Seldom, an operation might be needed to get rid of a clot from the lung.
Recovering From a Pulmonary Embolism
A pulmonary embolism (PE) is brought on by a blood clot that gets stuck in an artery in your lungs. That blockage can damage your lungs and harm other organs if they do not get enough oxygen. It’s a serious condition, and healing can take weeks or months.
When you’ve had one, your chances of another go up. But you can do some things to keep your blood flowing and prevent future embolisms. You’ll also wish to watch your legs for signs of a new members clot. Call your medical professional right away if you discover any of these:
- Swelling.
- Pain.
- Tenderness.
- Warmer-than-normal or red skin.
Diet and Medications
Drugs called anticoagulants are the first tools medical professionals grab if you’ve had a pulmonary embolism. They’re referred to as “blood thinners” because they make it harder for your blood to embolisms. They do not separate an embolism, but they keep it from growing as your body dissolves it.
When you take blood thinners, you’ll require to change what you consume. For example, foods rich in vitamin K, which helps your body kind embolism, might keep blood thinners from working like they should. That suggests you might require to consume fewer leafy green veggies and limit fish, liver, and some type of vegetable oil.
Ask your medical professional if it’s OKAY for you to consume alcohol while you take blood thinners.
You also ought to talk with your doctor about any other prescription or non-prescription medicines you take. Some common ones can affect how blood thinners work, too: These include:
- Aspirin.
- Cold medicines.
- Pain medicines.
- Sleeping tablets.
- Antibiotics.
You can anticipate to take blood thinners for a minimum of 3 months and potentially a lot longer. Some people require to take them for life.
Exercise
Most people can stroll and do light housework right now after a pulmonary embolism, but you may burn out quickly or feel short of breath.
Your doctor most likely will offer you particular workouts to do for a number of weeks or months to help improve your strength and breathing. Follow those recommendations, however don’t push yourself, especially if anything hurts or you discover any swelling.
Compression Stockings
A pulmonary embolism frequently starts in your legs, in one of the veins that brings blood to your heart and lungs. Making sure that blood flows freely can help avoid another blood clot.
One method to do that is with unique socks called compression stockings. These socks get tighter as they decrease toward your ankle, which helps your leg muscles move blood up your leg. Your physician will provide you a prescription for compression stockings that states how much pressure they need to apply.
Mental Health
This sort of severe, painful experience can leave you feeling unfortunate or afraid, specifically if your recovery puts new limitations on what you can do. If you feel distressed or depressed, talk with your physician about a referral to a counselor or support system in your area.
The Best Ways to Help Prevent a Blood Clots in Lung
When among the arteries that carries blood from your heart to your lungs gets obstructed, you have what physicians call a pulmonary embolism, or PE.
The majority of the time, this happens after an embolism kinds deep in a vein, typically in your leg. Physicians call this deep vein thrombosis, or DVT. If the clot breaks off and takes a trip to your lungs, it can block your blood circulation, triggering a PE.
The very best way to avoid a PE is to attempt to stop embolism from forming deep in your veins. This can be challenging if you’ve been on bed rest after a surgery or disease, or simply took a long flight. That’s since DVTs tend to form after you’ve been immobile for long periods of time.
If you’re at risk, here are five things that might help lower your opportunities of developing these harmful embolism:
Blood Thinners
Physicians call these “anticoagulants.” They keep your blood from forming embolisms. Your doctor might prescribe them to you while you’re in the medical facility for surgery. He may likewise suggest you keep taking them for some time after you go home.
Your physician might likewise suggest blood thinners if you’ve been hospitalized after a stroke or heart attack, or have complications from cancer.
Compression Stockings
These are long socks that squeeze your legs. The extra pressure helps blood relocation through your veins and leg muscles. Your doctor may recommend you wear them for a while after surgery.
Exercise
Get out of bed and walk when you’re getting over a long remain in the health center or a disease that’s kept you in bed for too long. It’ll keep the blood in your legs flowing so it doesn’t have a chance to pool.
Stretching During Trips
If you’re on a long flight, attempt to walk up and down the aisles every 30 minutes or two. If you can’t stand, flex your ankles by pulling your toes towards you.
Here’s another stretch you can try to do while seated:
- Pull your leg up toward your chest with one hand.
- Hold the bottom of that leg with the other hand.
- Keep this posture for 15 seconds, then attempt it with the other leg.
- Do this as much as 10 times per hour.
If you’re driving a long distance, stop every hour and stretch your legs.
Also, be sure to drink extra fluids to help you stay hydrated.
Way of life Changes
In addition to workout, there are a number of steps you can take moving forward. Here are some essential ones:
- Keep a healthy weight.
- If you plan to take hormonal agents, like birth control or replacement treatment, speak with your doctor about your risk for blood clots.
- If you have other health issues, like diabetes or cardiac arrest, take your medications, enjoy what you consume, and talk to your doctor about any changes.
- Also speak to your physician if you have a history of kidney disease or specific autoimmune diseases or a family history of blood clots.
- If you smoke, give up.
Q&A Regarding Pulmonary Embolism
How common is pulmonary embolism (PE) in kids?
DVT and pulmonary embolism are uncommon in pediatric practice. In 1993, David et al identified 308 kids reported in the medical literature from 1975-1993 with DVT of an extremity and/or pulmonary embolism. [16] In 1986, Bernstein reported 78 episodes of pulmonary embolism per 100,000 hospitalized adolescents. Unselected autopsy studies in kids approximate the occurrence of pulmonary embolism from 0.05-3.7%.
However, amongst pediatric patients in whom DVT or pulmonary emboli do happen, these conditions are related to considerable morbidity and death. Different authors suggest that pulmonary embolism adds to the death of afflicted kids in around 30% of cases. (Others, nevertheless, have actually reported pulmonary embolism as a cause of death in fewer than 5% of affected children.
Is pulmonary embolism (PE) more common in men or women?
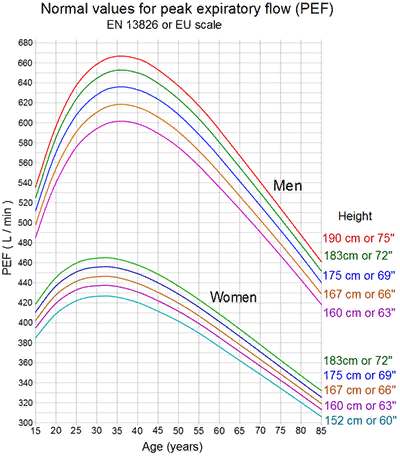
Data are contrasting as to whether male sex is a risk element for pulmonary embolism; however, an analysis of national death information found that death rates from pulmonary embolism were 20-30% greater amongst men than amongst women. The occurrence of venous thromboembolic occasions in the older population is greater among men than women. In patients younger than 55 years, the occurrence of pulmonary is higher in women. The overall age- and sex-adjusted yearly incidence of venous thromboembolism is reported to be 117 cases per 100,000 individuals (DVT, 48 cases per 100,000; pulmonary embolism, 69 cases per 100,000).
A potential cohort study of female nurses discovered an association between idiopathic pulmonary embolism and hours invested sitting each week. Women who reported in both 1988 and 1990 that they sat more than 40 hours weekly had more than two times the risk of pulmonary embolism compared to women who reported both years that they sat less than 10hours per week.
What is the incidence of pulmonary embolism (PE) in the US?
The occurrence of pulmonary embolism in the United States is estimated to be 1 case per 1000 individuals each year. Research studies from 2008 recommend that the increasing usage of computed tomography (CT) scanning for evaluating patients with possible pulmonary embolism has caused an increase in the reported occurrence of pulmonary embolism.
What is the role of long-lasting anticoagulation therapy for pulmonary embolism (PE)?
Long-term anticoagulation is critical to the prevention of recurrence of DVT or pulmonary embolism, because even in patients who are fully anticoagulated, DVT and pulmonary embolism can and frequently do recur.
Which thrombolytic agents are utilized in the treatment of pulmonary embolism (PE)?
Thrombolytic representatives utilized in handling pulmonary embolism consist of the following:
- Alteplase
- Reteplase
What is the difference in between central, peripheral, and massive pulmonary embolism (PE)?
A pulmonary embolism is also characterized as central or peripheral, depending upon the location or the arterial branch involved. Central vascular zones include the primary pulmonary artery, the left and right primary pulmonary arteries, the anterior trunk, the right and left interlobar arteries, the left upper lobe trunk, the right middle lobe artery, and the right and left lower lobe arteries. A pulmonary embolus is defined as enormous when it involves both pulmonary arteries or when it leads to hemodynamic compromise. Peripheral vascular zones include the segmental and subsegmental arteries of the right upper lobe, the right middle lobe, the right lower lobe, the left upper lobe, the lingula, and the left lower lobe.




Getting married triggered an embolism in my lungs.
If I had not gotten married, I would not have actually gone to Hawaii, Australia, New Zealand, Back to Australia, back to Hawaii for our honeymoon … investing a total of over 50 hours flying in coach while barely fitting in the seats at 6 ′ 7 ″. Not being able to move your legs on long flights is a bad thing. Plus it turns out I have a clotting condition, element V Leiden deficiency.
Anyhow, clots formed in my legs, traveled to my lungs, made me very short of breath -however I didn’t recognize what had actually taken place, so I didn’t go to the medical professional till other embolisms in my legs started getting truly agonizing.
I went to the center where they provided me a Doppler ultrasound test and found the embolisms. Next thing I understand I’m in an ambulance to the healthcare facility, where they offered me a CAT scan after I explained the shortness of breath symptoms. Later a medical professional came in, and with a somewhat shocked tone informed me I ‘d survived a bilateral pulmonary embolisms. I then spent week there on IV blood thinners.
Now I take rat toxin (warfarin) daily, and live every day like it’s my last.
Contact your physician ASAP. And it depends if its an internal or external clot. The medical professional can recommend a blood thinner like Warfarin or Coumadin, or he can put a shunt in your leg, or any place the clot is, to keep it from passing to your heart or lungs. However most significantly, you MUST keep your legs raised and stay off your part of the body where the clot is. Main idea is keep body or part of body like leg or arm elevated.
Pulmonary embolism is life threatening … if you make it through that, there is still the need to learn how poor the blood circulation remains in your legs that a clot established. That’s the mechanical side … find the rough spots where clots may occur.
Then there is the chemical side … Do you have lung damage or Lupus that can up the coagulation equation to the embolisms side? My laboratory buddy passed away from a small cancerous tumor in his lungs putting out coagulants … despite heparinization and a filter put in his vena cava, he passed away at home of another clot prior to he could begin his first chemo shot.
Lots of people most likely have embolisms in their lungs frequently, however, these are primarily microscopic.
A substantial embolism is one that will make a significant difference in the balance of ventilation to perfusion in the lung. This implies the quantity of the lung that has air and how this matches the flow of blood. Physiologically this indicates that the blood needs to have contact, across the membranes of the lung, to the air, so that we can take in oxygen and excrete carbon dioxide.
Because the entire flow in the body goes through the lungs a severe embolism can obstruct this, and cause death by blocking all flow. This is, in reality, how my 2nd partner died, a so-called saddle embolus. Death remains in seconds to minutes.
Smaller embolisms hinder the exchange of oxygen, making the individual feel “short of breath”. The person can not get enough oxygen. Carbon dioxide is not quite the concern at this stage.
Numerous episodes of pulmonary embolism, if not most, have NO premonitory symptoms.
A situation which can precede the advancement of embolisms in the lung is blood clotting in the legs. This may, but does not constantly, have symptoms. If there is inflammation or edema (swelling) in the legs there might be pain and swelling.
There are myriad other causes of embolism, a lot of which have no symptoms.
There usually is not any symptoms until it takes place. Definitely seek medical attention. Pulmonary Embolism (PE) generally starts as deep vein apoplexy (DVT). Many people get tiny embolisms every day, however the clot from DVT breaks off and travels to the lung. Signs can include shortness of breath, problems breathing, lightheadedness, and heavy sweating.
My coughing had actually not gone away despite a number of over-the-counter medications, the heaviness in my chest was also worsening. I had a 9 month old, 3 year old, and 13 years of age and my hubby was over 1000 miles away securing work and housing for the remaining 4 of us to join him within the next 2 to 3 months. We were sticking with a close family good friend and her kids. Things were tight but we made it work. On that last day of November I might no longer take this “chest cold” that had afflicted me for weeks. After a brief conversation with a pal, he concurred that I most likely needed an antibiotic and he and his sweetheart would provide me a ride to the medical facility near his house so that when I was done they could provide me a lift home. No one, however, was able to keep my 2 youngest kids, so an adventure took place! (My 13 years of age was at his father’s.).
The 3 people trepsed into the Emergency Department. It was loaded! I obviously checked in, met with the initial screener and quickly after my name was called. I was pleasantly suprised due to the amount of others in the waiting space, but hey, I wasn’t going to carry on. We were shown into what appeared to be an operating space. Perhaps where they carried out minor treatments when awaiting OR wasn’t an alternative. Needless to state after months of crashing on my friend’s couch the healthcare facility bed felt like paradise but the room itself held totally to numerous temptations for a curious 3 years of age and did nothing but piss off the 9 month old due to the fact that I would not enable her out of her provider to help her sister in the demolition that was bound to come.
After I was assessed by a nurse a physician came in, I duplicated myself for what seemed like the 10th time considering that I had existed. My medical history had seemed to take a bit longer than it used to. Adding 2 high risk pregnancies in the past 2.5 years, 2 more C-Sections, a diagnosis of Congestive Heart Failure when the last baby was hardly a week old due to 2 of my valves not working appropriately. Another diagnosis of serious Endometriosis that triggered a hysterectomy simply 30 days prior to the date of this ER visit. The hysterectomy surgery worked out and I was feeling much better but the healing from the surgery had actually been quite tough. I had wound up on home healthcare with an injury vac machine connected to my abdomen. It had become a total nightmare in itself and I was lastly machine free and tending to my cut by myself. This nasty chest thing was the last thing I wished to deal with. I was ill of physicians, tired of remaining in the medical facility, I just desired them to hurry up and compose me a ‘script for an antibiotic and let me and the now screaming banshees on our merry lil way. Obviously, not so quick, and naturally never that easy. Particularly when handling anything health associated for ‘moi. An X-Ray tech presented themselves with the duty to get images of my lungs. Great, I whispered to the youngsters. I felt in one’s bones with that added little service we would be encamping method past an acceptable supper time for my kiddos. I began to consider making phone calls to see about generating some dinner or perhaps getting someone to really take them for a little bit so that I might unwind, fill the prescription I was for sure getting, I suggest, they took X-Rays for goodness sake! And (gasp!) maybe even grab a bite to eat with some other adults !!
Just as I was scrolling through my contact list the doctor and the nurse came back squashing my dream of a meal that I didn’t prepare and did not consist of the words Happy Meal. My first thought was naturally getting my hot hands on whatever wonder drug the doc was going to prescribe to get this weight of a baby elephant off my chest, my doubt was, no warning. Now we will have to return to the cluster heap of the waiting space to wait on a ride outta there. I wasted no time at all, I started throwing little arms into coats and hats onto little heads asking the doctor simultaneously if it was bronchitis or possibly pneumonia and what medicine or medications was he going to prescribe to get me back to well, what was normal for me.
The nurse busied herself with my kids while the medical professional was advising me to please sit down. He then continued to ask me if there was a buddy or member of the family I might get in touch with to come pick up the ladies for me and keep them till more notice. I laughed off his remark, while some time off of mother duty sounded kinda good in a manner, there was actually no requirement to confess me for something like pneumonia or bronchitis. I guaranteed to take all my meds as recommended. The physician then very sternly notified me I was not being launched under any circumstances and I was dealing with a potentially lethal diagnosis. Well that sat me right down and shut me right up! The medical professional then informed me that after examining the x-ray films he found I had 11 pulmonary embolisms. When I was still sitting there with my mouth broad open he then described in layperson’s terms that I had 11 embolism in my lungs, 10 in my right lung and one in my left. Which I believed was strange because it was in fact the left side of my chest that was triggering the most pain. He explained that I would be admitted instantly and would be started on Heparin injections and would be begun on coumadin by mouth to get the blood clots to shrink in size and then ideally dissipate completely. I was frightened.
Here I was essentially a single mom with 3 kids. My other half was over a thousand miles away my mother was a number of hundred miles away my daddy and I were not close at all I had a bro that was close in distance but as far as our relationship goes we kind of do our own thing. He nevertheless was the first one I called he right away appeared and took my youngest daughter, my nine-month-old, with him for the night. My three-year-old was adamant that she was going to stay with me, here her daddy had actually been gone for four months, and now her mama was going to have to stay in the medical facility and she truly didn’t understand my sibling that well. Fortunately the healthcare facility consented to let her remain for one night till I might reach my mom and she could enter into town and acquire the children. The health center was very sweet, they comprised a little bed for her right beside mine total with blankets and sheets. Toys to play with appeared, coloring books, a set of pajamas it was actually good. I called my mom and she stated she would be there the next morning she had to do with a 4 hour drive away, I then called my kid’s dad and described the situation and of course him keeping my son was not an issue. I however for some factor could not reach my hubby who was down in San Antonio Texas while I was in St. Louis Missouri, but that’s for an entire another story.
As the ER physician expected I started Heparin injections right away and likewise was taking Coumadin twice-daily this went on for about 7 or 8 days with them doing x-rays on my chest every other day to check the size of the embolism. It took about a week of extensive anticoagulant therapy however the embolisms did soak up back into my body. I was to follow up with the Hematology group that looked after me in the healthcare facility. I continued the Heparin injections at home for about a week and rapidly became a regular at the “Coagulation Clinic” where for the first month or so I was subjected to weekly blood draws to identify the level my blood was clotting. The technical term is Proteome test. There was alot of adjusting of my medications and the awareness that I would be on blood thinners for the rest of my life.
So depending upon when the situation is caught and how aggressive the treatment is plays heavily on the prognosis of multiple embolism in the lungs. I consider myself to be very lucky to be alive today. Always err on the side of security. I am so happy I chose to go to the ER that tomorrow..
Hi I found out at the weekend that I had blood clots in both lungs. Has any else been diagnosed with this and how do you cope?
Yes, I have actually had multiple PE twice. The first time I was on warfarin for a year and then informed I wouldn’t require it anymore. Last May I had the second great deal of embolisms and have actually been told I will be on anticoagulants for life. I would be interested to understand whether you had DVT first or just PE.
Hi, Ryan! In my case, to deal with embolism in my lung, I was first given a bolus of heparin and then a couple of hours later on placed on a heparin drip IV. After 2 days I was switched to Coumadin and Lovenox.
I was enjoying TV when all of a sudden I could not breathe. I called 911 and when the emergency medical technician/paramedic inspected my EKG, he gave me an aspirin. In the emergency clinic I was poked and prodded. I was offered, among other drugs, morphine and nitroglycerin.
A professional came and drew more blood and I asked why and was informed that enzymes in my blood suggested I had, had a cardiac arrest. I was then sent to a heart unit in another health center where I was without delay removed of my clothes to all set me for surgery. A group of physicians began questioning me. I was a bit unclear on the pain in my chest due to the fact that I practically hurt all over.
A doctor pressed me very hard and out of confusion I offered up, ‘well, my leg has actually been troubling me for a long time, but I do not take note of aches (I’ve been operated on everywhere). An ultra noise was done of my leg, and a chest x-ray. After which I was not enabled to get up to go to the bathroom. I was told I had many clots in both lungs and lucky to be alive. After a 4 days in the cardiac intensive care unit I was sent home to administer my own shots in my abdomen.
Further blood tests revealed I had some type of hereditary defective gene that inclined me to DVTs (deep vein thromboses). I have actually now been on warfarin for many years and expect to remain on it for life.
I experienced unexpected shortness of breath but disregarded it for several days (very foolish). Lastly I went to the emergency room. D-dimer result was high, CAT scan showed bilateral pulmonary embolism and ultrasound revealed a DVT (deep vein apoplexy) in right leg. I was very lucky to have a cardiologist who had actually done a great deal of research study on using what he called safe dose thrombolysis. He utilized low dose TPA (tissue plasminogen activator) and within 3 hours my oxygen went from 86 to 98. No more shortness of breath and was released on Eliquis 5mg two times daily. It has been 3 months therefore far so good. I had no pain or swelling in my leg and no pain in my chest just the shortness of breath. Physicians called it an atypical case. Take shortness of breath seriously, it can save your life!
I’m a 37 year old female who has 4 embolism on my left lung. One is the size of a 50 cent piece. This is not my first time getting blood clots, I had pulmonary embolism 2 times before these ones. I took warfarin the first time for 7 months. They went away for not even 3 months and I started having discomforts again in my chest and finding it difficult to breathe. My medical professional told me to go to the emergency clinic (ER) and get a CAT scan done of my lungs and then they discovered I had 4 more embolism on my left lung. I’m told I’ll be on blood thinner warfarin for life. I needed to take injections in the stomach for 2 weeks, which made my stomach so aching and appearing like somebody beat me up. My stomach hurt to touch and even to take a seat. This is a very life threatening condition if you or anybody you understand have symptoms of having trouble in breathing, or if a touch or any part of your body seems like it is on fire, get to the ER and get medical assistance right now. If not it could cost you your life. These blood clots changed my life. I get brief of breath, it is hard to breathe and I pass out and can’t be active with my wife or kids due to not having the ability to breathe. To anyone who has this pulmonary embolism, I want you all the best.
My wife is 28 years of ages, she has brought to life our first child 3 weeks back. After one week she has actually struggled with extreme stabbing chest pain radiating to shoulder, increasing with motivation. There is no dyspnea, no cough, and no fever. To start with it was detected as muscular pain as the pain was alleviated by analgesics for a few hours, however the pain returns once again. X-ray was done and revealed mild pleural effusion, she was detected as having pleurisy, she got high doses of antibiotics and analgesics with no relief till the pulmonology physician recommended her to do CT angiography which revealed a little peripheral pulmonary arteriole embolism with infarcted area in lower lobe of right lung, D-dimer is high, double the normal, ESR is 115. Now she takes anticoagulant therapy (Clexane 80 every 12 hours, warfarin 5mg daily), antibiotic (clarithromycin 500mg 2 tabs daily) and analgesic.