There’s nothing quite as striking as an invisible enemy lurking within us, a sleeping giant that wakes up when we least expect it. One day we’re healthy, active individuals, and the next, we are fighting a battle with our own bodies.
This disguised “enemy” invades our nervous system unnoticed and causes dire consequences. This disease is real and leaves devastation in its wake. It’s called Guillain-Barre Syndrome, a rare disorder affecting thousands annually, and it remains shrouded in mystery to many.
We will bring medically accessible clarity to Guillain-Barré syndrome, examine the characteristic signs, and provide insight into the situations faced by those who have suffered this trouble.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Overview of Guillain-Barre Syndrome
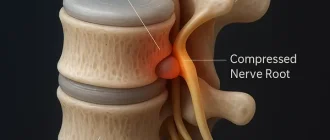
Guillain-Barre Syndrome (GBS) is a rare neurological disorder in which the body’s immune system mistakenly attacks the peripheral nerves, leading to weakness, tingling, and numbness in the extremities.
The exact cause of GBS remains unknown, but it often appears after a respiratory or digestive tract infection. Symptoms tend to worsen rapidly, potentially progressing to paralysis and causing difficulties in moving, walking, breathing, and swallowing.
Treatment for GBS typically includes intravenous immunoglobulin (IVIG) and plasma exchange to suppress the immune response, along with supportive care for symptom management. Most individuals recover from GBS within 6 to 12 months; however, some may experience long-term complications or even life-threatening issues.
Types of Guillain-Barre Syndrome
The most common subtype, Acute Inflammatory Demyelinating Polyneuropathy (AIDP), affects the glial cells surrounding the nerve axons, leading to sensory changes and muscle weakness.
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
In contrast, Acute Motor and Sensory Axonal Neuropathy (AMSAN) involves the direct attack on nerve axons, with more aggressive symptoms and longer recovery periods.
Another variant, Acute Motor Axonal Neuropathy (AMAN), specifically targets nerves controlling movement, resulting in weakness without numbness.
Lastly, the rare Miller-Fisher Syndrome (MFS) exhibits unique symptoms such as eye muscle paralysis and loss of balance coordination.
Proper identification of GBS types enables healthcare professionals to administer appropriate treatments, including plasmapheresis and intravenous immunoglobulins, which can significantly improve patient outcomes.
Symptoms and Warning Signs
- Tingling sensations: Patients often experience a pins and needles sensation in their fingers, toes, ankles, or wrists, which can be the first sign of the syndrome.
- Muscle weakness: This starts in the legs and spreads to the upper body, affecting the arms and face in later stages.
- Unsteady walking: Patients may struggle to walk or climb stairs due to muscle weakness.
- Facial movement difficulties: Speaking, chewing, and swallowing can be difficult due to affected facial muscles.
- Double vision or eye movement issues: Patients may experience problems with their vision and controlling eye movements.
- Severe pain: This can feel achy, shooting, or cramp-like, and may worsen at night.
- Loss of bladder or bowel control: This can occur as the syndrome progresses.
- Breathing difficulty: In severe cases, Guillain-Barre Syndrome can impact the ability to breathe, which is a medical emergency.
Causes of Guillain-Barre Syndrome
Guillain-Barre Syndrome (GBS) is a rare, autoimmune disorder characterized by an attack on the peripheral nervous system, leading to symptoms such as tingling, muscle weakness, and even paralysis in severe cases.
Although the exact cause of GBS is still unknown, it often appears days or weeks following a respiratory or digestive tract infection. Certain surgeries and vaccinations have also been linked to triggering GBS.
In some instances, the Zika virus infection has been associated with this syndrome. While the precise mechanism leading to GBS remains unclear, understanding the potential causes and triggers can help guide appropriate medical intervention and management.
Risk Factors Associated with Guillain-Barre Syndrome
The exact cause of GBS remains unknown, but it usually occurs after a respiratory or digestive tract infection, surgery, or vaccination. Some reported cases have also been linked to the Zika virus.
Risk factors associated with GBS severity include a recent history of surgery, older age, cranial nerve impairment, and elevated levels of liver enzymes. It is crucial to identify these risk factors at an early stage to determine the appropriate therapeutic method and predict short-term prognosis in patients with severe GBS.
Diagnosis
Diagnosing Guillain-Barre syndrome can be challenging, particularly in its early stages, as its signs and symptoms resemble those of other neurological disorders and vary from person to person.
A comprehensive diagnosis typically begins with a medical history assessment and a thorough physical examination. Two specialized tests are conducted to assess nerve functionality: electromyography (EMG) and nerve conduction studies.
Additionally, a lumbar puncture may be performed to obtain a sample of cerebrospinal fluid, which helps in identifying any infections that may cause similar symptoms to Guillain-Barre syndrome. The accurate diagnosis of this condition is vital to ensure proper treatment and management for a successful recovery.
Treatment Options
Dealing with a diagnosis of Guillain-Barre Syndrome (GBS) can be challenging, but understanding the treatment options can ease the stress. Here’s a quick guide on how to manage GBS treatments:
- Consult your doctor for a thorough examination, diagnosis, and treatment recommendation.
- Know the standard treatment options for GBS: Plasmapheresis, which removes and replaces plasma from the blood, and Intravenous Immunoglobulin Therapy, which adds healthy antibodies to the bloodstream. Both treatments aim to reduce the severity and speed up the recovery process.
- Be aware that medication may be prescribed to relieve pain, prevent blood clots, and manage other symptoms.
- Embrace physical therapy sessions to help strengthen muscles, regain movement, and learn adaptive techniques for mobility and self-care.
- Stay in close communication with healthcare professionals and support networks throughout the recovery process, which may take months or even years.
Remember, most GBS patients experience a full recovery with the right treatment and support system.
Prevention
Preventing Guillain-Barre Syndrome (GBS) can be challenging, as the exact cause remains unknown. However, understanding the risk factors and maintaining a healthy lifestyle could potentially lower one’s likelihood of developing the condition.
Since GBS is often triggered by a viral or bacterial infection, practicing good hygiene and getting vaccinations can help prevent these infections and possibly minimize the risk of GBS. Handling food properly, avoiding contaminated water, and seeking prompt treatment for any illness may also contribute to prevention efforts.
It is essential to talk to your healthcare provider about your concerns, as there is no one-size-fits-all solution for GBS prevention.
Prognosis and Recovery
Guillain-Barre Syndrome (GBS) is a condition that affects the peripheral nervous system and can be challenging to diagnose and manage. While there is no cure, treatments such as plasmapheresis and intravenous immunoglobulin can aid in recovery and reduce the severity of the illness.
Long-term prognosis varies, with 80% of adults able to walk independently six months after diagnosis and 60% fully recovering motor strength after one year.
In some cases, it may take as long as three years for complete recovery. It is important for GBS patients to maintain a strong support system, engage in physical therapy, and work closely with healthcare professionals to manage the condition effectively.