To identify the clinical outcome and medical statistic of survival after transjugular intrahepatic portosystemic stent shunt (TIPS) implantation in cirrhotic patients.
What is TIPS?
A transjugular intrahepatic portosystemic shunt (TIPS) is a tract developed within the liver utilizing x-ray assistance to connect 2 veins within the liver. The shunt is kept open by the positioning of a little, tubular metal device typically called a stent.
During a TIPS treatment, interventional radiologists utilize image assistance to make a tunnel through the liver to connect the portal vein (the vein that brings blood from the gastrointestinal organs to the liver) to among the hepatic veins (three veins that bring blood away from the liver back to the heart). A stent is then placed in this tunnel to keep the path open.
Health Support: This Vitamin K2 + D3 Complex is essential for bone density, cardiovascular health, and immune function. It’s a highly-rated formula for those looking to maintain optimal nutrient levels. You can find it on Amazon.
Patients who typically require a TIPS have portal high blood pressure, indicating they have increased pressure in the portal vein system. This pressure buildup can trigger blood to flow backward from the liver into the veins of the spleen, stomach, lower esophagus, and intestines, causing enlarged vessels, bleeding and the build-up of fluid in the chest or abdominal area. This condition is most typically seen in adults, frequently as a result of chronic liver problems resulting in cirrhosis (scarring of the liver). Portal high blood pressure can also occur in children, although kids are much less most likely to require a TIPS.
See also: Hepatitis C and Liver Cancer
Survival Rates after Transjugular Intrahepatic Portosystemic Stent Shunt Procedure
Here is average life expectancy stat for patients who got TIPS procedure:
88% of patients
Health Support: This high-absorption Magnesium Glycinate (200 mg) is gentle on the stomach and supports muscle relaxation, better sleep, and metabolic health. You can find this trusted formula on Amazon.
61%
2+ yrs
5+ yrs
How long can you live after a TIPS procedure if you have complications?
Survival rates (Kaplan-Meier) of the overall mate were 63%, 56%, 39%, and 29% after 3, 6, 12, and 18 months, respectively, with a mean survival of 75 (14) weeks (95% CI 48 — 102, median 34). TIPS patients showed substantially better survival than non-TIPS patients with advanced liver dysfunction at baseline.
After TIPS, 3, 6, 12, and 18 month survival rates were 81%, 71%, 48%, and 35% (mean survival 92 (16) weeks; 95% CI 60 — 123; median 49) compared with non-TIPS patients (3 month survival of 10% and a mean survival of 12 (8.5) weeks (95% CI 0.01– 28; median 2.0)).
Type II HRS patients had a much better possibility of survival than type I patients. TIPS patients whose ascites were mobilised within one month (clinical responder) endured longer than patients who did not respond. Interestingly, even type I patients treated with TIPS (n=14) attained 3, 6, and 12 month survival rates of 64%, 50%, and 20%, which were significantly much better than the survival rates of type I patients who did not go through TIPS with similar kidney dysfunction at baseline.
Integrated survival analysis of all 21 type I HRS patients revealed 3, six, and 12 month survival rates of 48%, 38%, and 16% (Kaplan-Meier plot not shown).
What is Prurigo Nodularis?
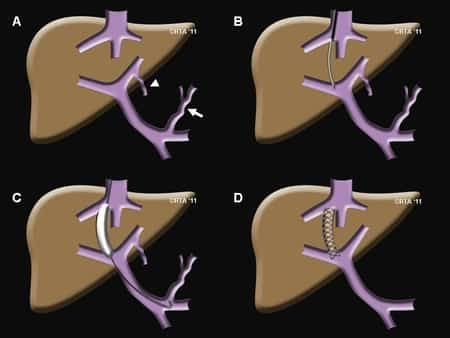
TIPS for Cirrhosis
A TIPS procedure might be done by a radiologist, who puts a small wire-mesh coil (stent) into a liver vein. The stent is then expanded using a little inflatable balloon (angioplasty). The stent types a channel, or shunt, that bypasses the liver. This channel reduces pressure in the portal vein. By lowering portal high blood pressure, enlarged veins (varices) are less most likely to burst and bleed. And other issues of cirrhosis called ascites (fluid in the abdominal area) and hepatic hydrothorax (fluid in between the lungs and the chest wall) may enhance or go away.
TIPS may be used to:
- Treat fluid buildup that continues to take place in the stomach cavity regardless of medical therapy (refractory ascites).
- Deal with acute variceal bleeding that is not controlled by standard treatment.
- Prevent reoccurring episodes of variceal bleeding when sclerotherapy or band ligation has stopped working.
- Treat variceal bleeding while somebody is waiting for a liver transplant.
Complications of the procedure may include:
- Encephalopathy. Up to 20 out of 100 people who have TIPS surgery establish encephalopathy after the surgery.
- Malfunction of the stent, such as narrowing (stenosis) or closing (occlusion).
How Long Do Liver Stents Last?
The mean duration of the patency of the stent has to do with 12 months. The biliary stenting is performed either with plastic or metal stents, studies recommending their replacement after 3-6 months. Patients with long remained forgotten biliary stents are inevitably treated with surgical intervention.
See also: Low Liver Enzymes
Side Effects and Possible Risk during or after the Procedure
Possible risks with this procedure are:
- Damage to blood vessels
- Fever
- Hepatic encephalopathy (a disorder that affects concentration, mental function, and memory, and may result in coma).
- Infection, bruising, or bleeding.
- Responses to medicines or the color.
- Stiffness, bruising, or pain in the neck.
Uncommon threats are:
- Bleeding in the belly.
- Obstruction in the stent.
- Cutting of blood vessels in the liver.
- Heart problems or irregular heart rhythms.
- Infection of the stent.